Chronic hep B and the liver
Indication and Important Safety Information

What is hep b?
Chronic hepatitis B (hep B) is a disease caused by long-term infection by the hepatitis B virus. Over time, it can lead to serious liver damage.
It's important to know that you can’t get hepatitis B from touching, kissing, drinking alcohol, food, water, air, or sharing cups and utensils.
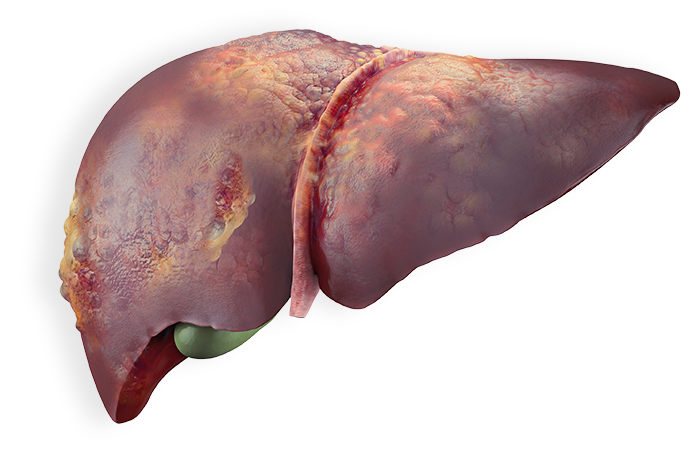
WHAT DOES THE LIVER DO?
The liver is one of the most important parts of the body. It does a lot of things that help you every day, including:




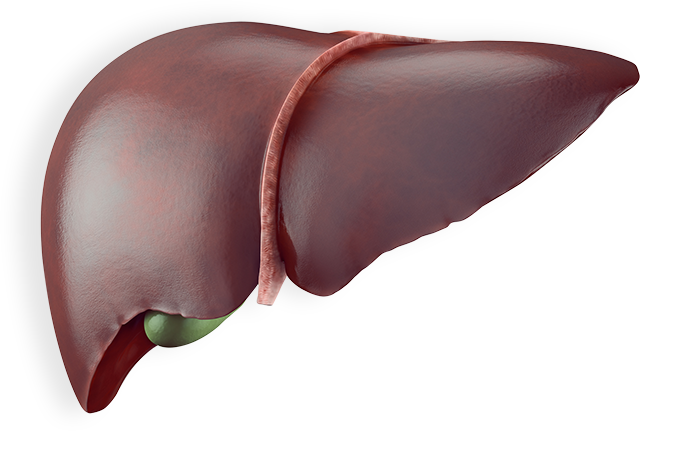
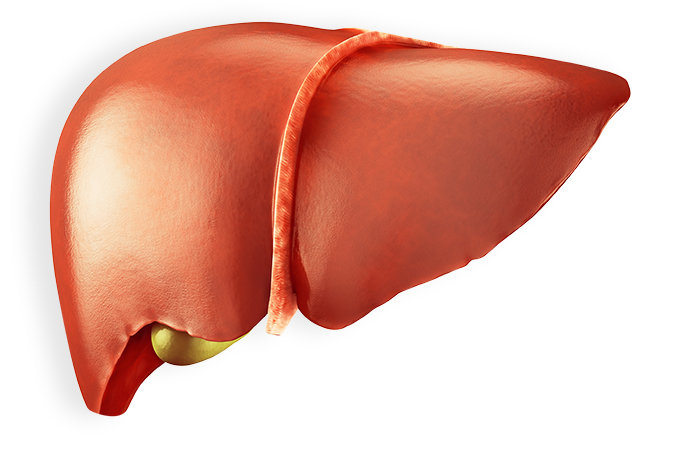
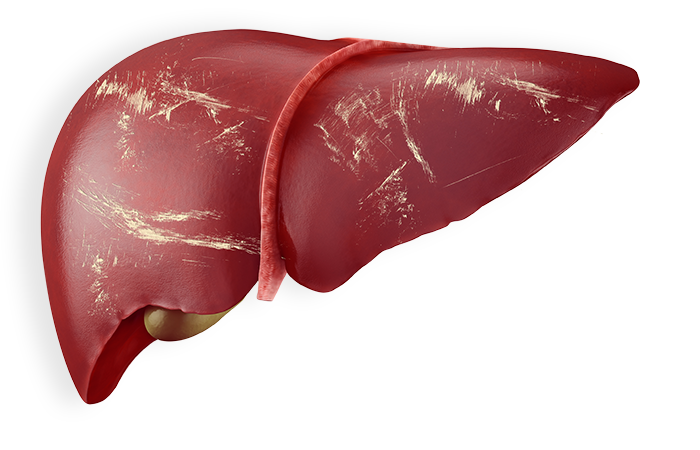
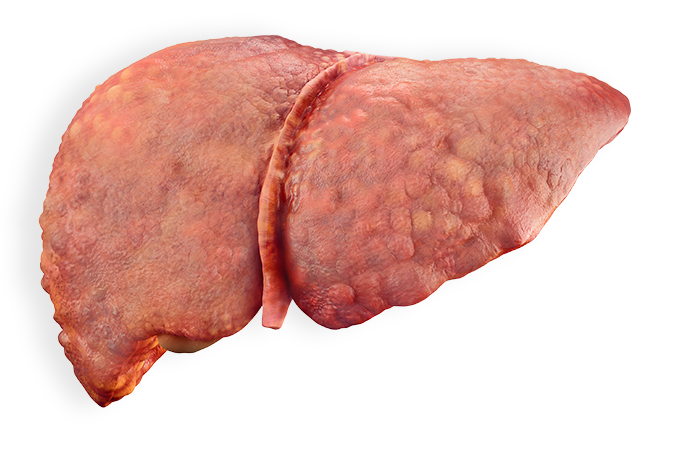
How chronic hepatitis B can damage the liver
The longer you have hepatitis B, the more damage it can cause. Because of the risk for severe liver damage, it is important to see your doctor regularly, even if you feel fine.
Chronic hepatitis B can lead to:
What is VEMLIDY?
VEMLIDY is a prescription medicine used to treat chronic (long-lasting) hepatitis B virus (HBV) in adults with stable (compensated) liver disease.
- VEMLIDY may lower the amount of HBV in your body.
- VEMLIDY may improve the condition of your liver.
What is the most important information I should know about VEMLIDY?
VEMLIDY can cause serious side effects, including:
- Worsening of hepatitis B virus (HBV) infection. Your HBV infection may get worse (flare-up) if you take VEMLIDY and then stop taking it. A “flare-up” is when your HBV infection suddenly returns in a worse way than before. Do not stop taking VEMLIDY without first talking to your healthcare provider, as they will need to monitor your health regularly to check your liver.
What should I tell my healthcare provider before taking VEMLIDY?
All of your medical conditions, including if you have end stage renal disease (ESRD) or HIV-1 infection. Your healthcare provider may test you for HIV infection before starting VEMLIDY. If you have HIV and only take VEMLIDY, the HIV virus may develop resistance and become harder to treat.
If you are pregnant or plan to become pregnant. It is not known if VEMLIDY will harm your unborn baby. Tell your healthcare provider if you become pregnant during treatment with VEMLIDY.
If you are breastfeeding or plan to breastfeed. VEMLIDY may pass into your breast milk. Talk with your healthcare provider about the best way to feed your baby.
Continued below
What are the symptoms?
important safety information (continued)
If you feel any of the following hep B symptoms, do not ignore them and make sure to tell your doctor immediately. He or she will do tests to see if it is hep B-related.
Hepatitis B symptoms may include:








Many patients with chronic hepatitis B do not experience any symptoms. Even if you don't feel any symptoms, the hepatitis B virus is still in your body and may be harming your liver
What should I tell my healthcare provider before taking VEMLIDY? (continued)
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Some medicines may affect how VEMLIDY works. Keep a list of all your medicines and show it to your healthcare provider and pharmacist. Do not start a new medicine without telling your healthcare provider. Ask your healthcare provider if it is safe to take VEMLIDY with all of your other medicines.
What are the possible side effects of VEMLIDY?
- New or worse kidney problems, including kidney failure. Your healthcare provider should do blood and urine tests to check your kidneys when starting and during treatment with VEMLIDY. Your healthcare provider may tell you to stop taking VEMLIDY if you develop new or worse kidney problems.
- Too much lactic acid in your blood (lactic acidosis), which is a serious but rare medical emergency that can lead to death. Tell your healthcare provider right away if you get these symptoms: weakness or being more tired than usual, unusual muscle pain, being short of breath or fast breathing, stomach pain with nausea and vomiting, cold or blue hands and feet, feeling dizzy or lightheaded, or a fast or abnormal heartbeat.
Continued below
The goal of HBV treatment
important safety information (continued)


The goal of prescription medicine is to:

Decrease the amount
of virus in the body

Reduce the risk
of liver damage
If you are currently on treatment, there are tests that can tell how well your medicine is working. Talk to your doctor about why these tests are important and how to schedule them.
What are the possible side effects of VEMLIDY? (continued)
- Severe liver problems, which in rare cases can lead to death. Tell your healthcare provider right away if you get these symptoms: skin or the white part of your eyes turns yellow, dark “tea-colored” urine, light-colored stools, loss of appetite for several days or longer, nausea, or stomach-area pain.
The most common side effect of VEMLIDY is headache.
These are not all the possible side effects of VEMLIDY. Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
Click here for Important Facts about VEMLIDY, including important warnings.
History of chronic hep B treatment
Indication and Important Safety Information
Timeline of FDA Approvals: Oral Antiviral Treatments for Chronic Hep B

This timeline is not intended to compare the efficacy or safety of the products listed above.
Talk to your doctor to determine which treatment is right for you.
What is VEMLIDY?
VEMLIDY is a prescription medicine used to treat chronic (long-lasting) hepatitis B virus (HBV) in adults with stable (compensated) liver disease.
- VEMLIDY may lower the amount of HBV in your body.
- VEMLIDY may improve the condition of your liver.
Continued below
Important Safety Information
What is the most important information I should know about VEMLIDY?
VEMLIDY can cause serious side effects, including:
- Worsening of hepatitis B virus (HBV) infection. Your HBV infection may get worse (flare-up) if you take VEMLIDY and then stop taking it. A “flare-up” is when your HBV infection suddenly returns in a worse way than before. Do not stop taking VEMLIDY without first talking to your healthcare provider, as they will need to monitor your health regularly to check your liver.
What should I tell my healthcare provider before taking VEMLIDY?
All of your medical conditions, including if you have end stage renal disease (ESRD) or HIV-1 infection. Your healthcare provider may test you for HIV infection before starting VEMLIDY. If you have HIV and only take VEMLIDY, the HIV virus may develop resistance and become harder to treat.
If you are pregnant or plan to become pregnant. It is not known if VEMLIDY will harm your unborn baby. Tell your healthcare provider if you become pregnant during treatment with VEMLIDY.
If you are breastfeeding or plan to breastfeed. VEMLIDY may pass into your breast milk. Talk with your healthcare provider about the best way to feed your baby.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Some medicines may affect how VEMLIDY works. Keep a list of all your medicines and show it to your healthcare provider and pharmacist. Do not start a new medicine without telling your healthcare provider. Ask your healthcare provider if it is safe to take VEMLIDY with all of your other medicines.
What are the possible side effects of VEMLIDY?
- New or worse kidney problems, including kidney failure. Your healthcare provider should do blood and urine tests to check your kidneys when starting and during treatment with VEMLIDY. Your healthcare provider may tell you to stop taking VEMLIDY if you develop new or worse kidney problems.
- Too much lactic acid in your blood (lactic acidosis), which is a serious but rare medical emergency that can lead to death. Tell your healthcare provider right away if you get these symptoms: weakness or being more tired than usual, unusual muscle pain, being short of breath or fast breathing, stomach pain with nausea and vomiting, cold or blue hands and feet, feeling dizzy or lightheaded, or a fast or abnormal heartbeat.
- Severe liver problems, which in rare cases can lead to death. Tell your healthcare provider right away if you get these symptoms: skin or the white part of your eyes turns yellow, dark “tea-colored” urine, light-colored stools, loss of appetite for several days or longer, nausea, or stomach-area pain.
The most common side effect of VEMLIDY is headache.
These are not all the possible side effects of VEMLIDY. Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
Click here for Important Facts about VEMLIDY, including important warnings.
Indication and Important Safety Information
What is vemlidy?
VEMLIDY is a prescription medicine used to treat chronic (long-lasting) hepatitis B virus (HBV) in adults with stable (compensated) liver disease.
- VEMLIDY may lower the amount of HBV in your body.
- VEMLIDY may improve the condition of your liver.
What is the most important information I should know about VEMLIDY?
VEMLIDY can cause serious side effects, including:
- Worsening of hepatitis B virus (HBV) infection. Your HBV infection may get worse (flare-up) if you take VEMLIDY and then stop taking it. A “flare-up” is when your HBV infection suddenly returns in a worse way than before. Do not stop taking VEMLIDY without first talking to your healthcare provider, as they will need to monitor your health regularly to check your liver.
What should I tell my healthcare provider before taking VEMLIDY?
All of your medical conditions, including if you have end stage renal disease (ESRD) or HIV-1 infection. Your healthcare provider may test you for HIV infection before starting VEMLIDY. If you have HIV and only take VEMLIDY, the HIV virus may develop resistance and become harder to treat.
If you are pregnant or plan to become pregnant. It is not known if VEMLIDY will harm your unborn baby. Tell your healthcare provider if you become pregnant during treatment with VEMLIDY.
If you are breastfeeding or plan to breastfeed. VEMLIDY may pass into your breast milk. Talk with your healthcare provider about the best way to feed your baby.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Some medicines may affect how VEMLIDY works. Keep a list of all your medicines and show it to your healthcare provider and pharmacist. Do not start a new medicine without telling your healthcare provider. Ask your healthcare provider if it is safe to take VEMLIDY with all of your other medicines.
What are the possible side effects of VEMLIDY?
- New or worse kidney problems, including kidney failure. Your healthcare provider should do blood and urine tests to check your kidneys when starting and during treatment with VEMLIDY. Your healthcare provider may tell you to stop taking VEMLIDY if you develop new or worse kidney problems.
- Too much lactic acid in your blood (lactic acidosis), which is a serious but rare medical emergency that can lead to death. Tell your healthcare provider right away if you get these symptoms: weakness or being more tired than usual, unusual muscle pain, being short of breath or fast breathing, stomach pain with nausea and vomiting, cold or blue hands and feet, feeling dizzy or lightheaded, or a fast or abnormal heartbeat.
- Severe liver problems, which in rare cases can lead to death. Tell your healthcare provider right away if you get these symptoms: skin or the white part of your eyes turns yellow, dark “tea-colored” urine, light-colored stools, loss of appetite for several days or longer, nausea, or stomach-area pain.
The most common side effect of VEMLIDY is headache.
These are not all the possible side effects of VEMLIDY. Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
Click here for Important Facts about VEMLIDY, including important warnings.
Tap for Indication and Important Safety Information, including important warnings on worsening of hepatitis B infection.